The LNP Mystery Part III
A look at the "Highly Inflammatory" study, and things to consider with LNPs.
I thought it would be rather fitting to round out the LNP talk (at least for now) with a look at the “Highly Inflammatory” study from Ndeupen et. al. as it may help to tie together some of the different perspectives of these LNPs.
This study was in preprint form in early 2021. However, this is the full release of the study.
Now, before we get into it we must keep in mind a rather important aspect of inflammation. For all of our discussions of inflammation, we may ascribe a negative connotation to the role of inflammation in physiology. It’s certainly true that most examinations of disease now take into account the role of inflammation, especially in diseases such as autoimmune disease, obesity, and diabetes.
But inflammation is also a necessary part of dealing with damage to the body. It’s part of the healing process when we receive cuts and bruises, and we experience inflammation when the immune system must deal with a pathogen that has made its way into our bodies.
In general, inflammation is vital to our well-being and survival. It is only when the inflammation we experience persists for far too long, or occurs when it is not necessary. Keep this in mind when we review the “Highly Inflammatory” article.
The mRNA-LNP platform’s lipid nanoparticle component used in preclinical vaccine studies is highly inflammatory (Ndeupen et. al.)
Considering that the ionizable lipids used in the mRNA vaccines were considered to be safer than their quaternary counterparts, the researchers of this study wanted to examine the inflammatory effects of the ionizable lipids alone using mice models.
The ionizable lipids were developed to decrease the highly inflammatory and cytotoxic effects of some of the permanently charged cationic lipids (Kulkarni et al., 2018). A preclinical study showed that nucleoside-modified mRNA complexed with Acuitas Therapeutics' LNPs containing proprietary ionizable lipid has adjuvant activity (Pardi et al., 2018a). However, the potential inflammatory nature of these LNPs was not assessed (Alameh et al., 2020; Pardi et al., 2018a).
Now, compared to other studies this one was rather straightforward and short, so I encourage people read the study since it would not be too difficult to analyze.
The researchers looked specifically at Acuitas’ ionizable lipid1, although they don’t actually indicate the structure of the lipids used in their studies (refer to Footnote 1).
Mice were injected either intradermally (within the skin tissue; 4 separate spots at 2.5ug mRNA/LNP each) or intramuscularly (within the muscle; 10ug mRNA/LNP) The researchers also conducted another study examining intranasal vaccination as another possible route, especially since intranasal COVID vaccines are currently being examined. Tissue samples were collected and analyzed for inflammation.
Inflammation after Intradermal/Intramuscular Injection
As expected, inflammation- by virtue of examining muscle tissue as well as biomarkers- indicated local inflammation and an influx of leukocytes and neutrophils when administered ionizable lipids versus control or a nonionizable lipid vector.
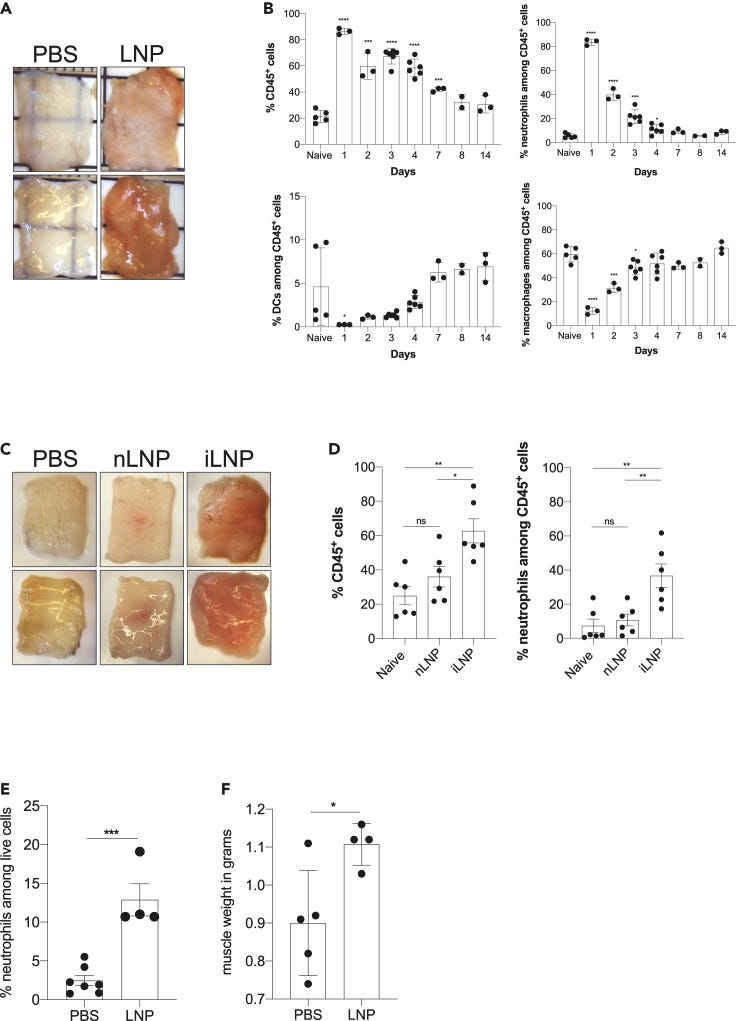
The researchers commented:
In summary, using different techniques, we show that LNPs, alone or complexed with control noncoding poly-cytosine mRNA, are highly inflammatory in mice, likely through the engagement and activation of various distinct and convergent inflammatory pathways.
So the results of these experiments point to the ionizable lipids as being inflammatory. The LNP that lacked ionizable lipids did not exhibit the same level of inflammation. However, if the researchers replaced the ionizable lipids without other platforms was not necessarily mentioned, and so whether these lipids contained quaternary amines or another lipid is up for debate.
Inflammation after Intranasal Vaccination
In order to see whether route of administration played a role in local inflammation, the researchers provided different doses of ionizable lipid-based LNP intranasally to mice and examined their effects. The idea here is to see if LNP accumulation within the lungs may cause inflammation. In general, there was a dose-dependent relationship seen, such that higher doses of LNP led to higher rates of inflammation of lung tissue. In fact, many of the mice at the higher (10ug) dose died during the study.

Taken together, these experiments suggest that the ionizable lipids are inflammatory, and may lead to local inflammation based on the inflammation seen in the muscle tissue as well as the lungs.
Examining the Results
So, at this point we may need to take into account that small remark I made at the beginning about inflammation, and also explain a few problems I have with this study.
When we look at the role of inflammation with respect to vaccination, this type of inflammation may not be bad. Actually, this type of inflammation may aid in immune response and boost a response to the spike protein. The researchers in this study comment that they believe this type of local inflammation allows the ionizable lipids to serve as adjuvants:
Here we show that the LNPs used for many preclinical studies (Freyn et al., 2020; Laczkó et al., 2020; Lederer et al., 2020; Pardi et al., 2017, Pardi et al., 2018a, Pardi et al., 2018b) are highly inflammatory. This could explain their potent adjuvant activity and their superiority, compared with other adjuvants, in supporting the induction of adaptive immune responses.
Previous preclinical mouse data suggested that mRNA complexed with LNPs have adjuvant activity (Pardi et al., 2018a). The mRNA is nucleoside modified and purified to decrease activation of certain innate inflammatory pathways (Karikó et al., 2005; Karikó et al., 2008, 2011). Our injection-site-focused analyses revealed the inflammatory nature of these LNPs, which likely provides a basis for their adjuvant properties.
Now, if you read just the title and the abstract, you probably would not have assumed that this is the conclusion to take away. People who have reported on this paper referred to the inflammation as being dangerous, yet the authors beat around the bush on that argument.
The researchers mention side effects, which many of us may take to refer to myocarditis or other serious risks, yet the researchers here refer specifically to pain, swelling, fever and sleepiness when discussing side effects. Why refer to the smaller side effects, and not the greater concerning features?
They do make a few interesting comments about the lipids buried within the Discussion section:
The synthetic ionizable lipid in the Pfizer SARS-CoV-2 vaccine has been speculated to have approximately 20–30 days of half-life in humans (Comirnaty, 2021). Whether the long-term presence of ionizable lipid could lead to low levels of chronic inflammation and immune exhaustion (Wherry and Kurachi, 2015) remain to be determined.
To the extent that these LNPs are long-lived, I am unsure, but I find it interesting that some of the more concerning features of the LNPs were buried within the Discussion section rather than included within the analysis of the information, including a minor remark about LNPs being found within the CNS but downplayed for existing in trace amounts and likely not to cause severe inflammation. Again, I suggest people read the discussion, including the section on possible reasons for booster side effects.
Some Takeaways
So what should we take away from this study? It’s a decent study in measuring local inflammation after administration of ionizable lipids, although I still don’t know which lipids were used in this study- maybe one of you can figure it out.
What’s more important is the intranasal experiment, which indicates that high exposure in the lungs and excessive inflammation can be extremely harmful. Considering that we know the LNPs can travel, this may at least suggest that the LNPs can be involved with systemic inflammation. Also, depending upon which organs uptake the LNPs there may be concerns about inflammation of certain organs and vital tissues. Remember, we are unsure of how much LNPs are actually travelling as no studies to date actually quantified this amount.
It’s rather interesting that the researchers only speculated to inflammation of the hypothalamus and intranasal vaccination using only the symptoms of the mice instead of examining their CNS for signs of inflammation. In fact, it feels as if the researchers could have done a lot more to examine systemic inflammation by measuring other organs and serum for various pro-inflammatory biomarkers. Why was this not done? I’ll leave it for others to speculate, but I suppose we may have some plausible reasons as to what may be going on.2
Things to Consider
To put it lightly, I may have had a change of heart of these lipids. Not to the extent that I believe them to be highly toxic, but more than they are not such an innocent bystander. I’m willing to believe that many of the adverse reactions we are seeing may be tied to the spike protein and even other goings on, but the lipids may also be a contributing factor. There is plenty of evidence of the LNPs being pro-inflammatory, although to the extent that this is playing out in humans is yet to be determined.
So here’s a few ideas I’ve been thinking about, and things that may be worth considering when examining these lipids:
The site of inflammation is important. This isn’t some revelatory idea, but just to emphasize this point- inflammation in general is not an issue. Local inflammation is likely to serve as an aid in immune response, and in that regard it may be beneficial when intending to elicit an immune response. The issue is when the inflammatory agent may widely distribute and move outside of the initially intended scope. We know that these lipids don’t stay in one place, so the important issue is how much of them escape, and where these lipids are ending up. This also may raise questions as to routes of administration of these vaccines. Early questions about SARS-COV2’s infection pathway suggested possible neuroinvasion through the olfactory bulb, which should raise questions about the accessibility of the CNS to the LNPs if vaccines are administered intranasally.
The “sponging” effect: This is another unoriginal idea that has circulated around for some time (no pun intended). I first came across it somewhere on Substack, in which someone linked to a Tweet that suggested elderly people experienced fewer adverse reactions due to the high lipid content of their blood and tissues (i.e. old people tend to be fat). I didn’t pay much mind to the Tweet at the time, but it’s made me rather curious about if there may be some truth in that assessment. Essentially, people who are fatter may have a greater “barrier of entry” for these vaccines to get into into vital organs and tissues. Their higher lipid count may serve as a “sponge” and absorb the LNPs. This still seems like a farfetched idea to me, but it would be interesting to see if stratified data for BMI may indicate possible adverse reaction signals between those with higher BMI and lower BMI. This may (emphasis MAY) explain the current issues with athletes. There may be a selection bias at play as well, but considering that many of the athletes that appear to be collapsing are endurance athletes such as soccer and basketball players, there may be some basis for leaner athletes being more susceptible to adverse reactions. Again, this is very likely not a new idea and may be more speculative than anything, but it would be rather interesting to see some possible correlation.
What is the fate of the lipids? Dr. Malone’s early remarks of these cationic lipids suggested that they fused to the cell’s membranes and spewed their mRNA guts into the cell, similar to the membrane fusion route of SARS-COV2. However, most studies of these LNPs suggest that they follow the endocytic route of entry, meaning that they are taken up by endosomes, and due to the highly acidic environment the lipids break up and release the mRNA which escapes into the cytosol. That’s all well and good, but the issue is what happens to the lipids after the mRNA is released? Do they remain within the endosomes and degrade due to the acidic environment and endosomal lipases3, or could they possibly reassemble into liposomes? The latter should not be dismissed since the lipids are known to self-assemble. In that case, is it likely that cellular havoc due to forced production of the spike protein may allow for escape of the empty liposomes into the extracellular environment?
Multi-Factorial Toxicity: In general, if we are to believe that minor traces of the LNP will circulate in the body, the possible inflammation may be kept to a minimal. However, these LNPs may not exist in isolation- the are likely to be carriers of the spike mRNA and thus may lead to the production of the spike protein with its own toxicities. Think of a scenario where a few of the LNPs may make their way to the heart. The LNPs may cause minor inflammation within the environment, but the cells that take up the LNPs are given the “kiss of death” and thus must be forced to manufacture the spike, causing another separate inflammatory process. The end result is a spike protein targeted by the immune system, leading to cell death and possible release of the spike into the environment which leads to further inflammation and cytotoxicity. Taken altogether, what may make these vaccines unique is that each individual component may contribute to inflammation and cytotoxicity, and it could be the combination of all components that make these vaccines so toxic. It is likely to not be one component alone, but all components and the overall process that is contributing to the detrimental effects we are seeing. Current studies may take an either/or approach, rather than take a holistic approach and view the entire process as a whole. I’ll elaborate more on this topic when discussing the Adenoviral vector vaccines later in the week and how this is likely occurring with those vaccines.
This may be it for now with the haphazard LNP assessment, but if anyone has any questions, comments, or criticisms please comment below!
Although we may assume it is ALC-0315 that was used in this study, the researchers don’t clarify which LNP was used aside from a comment referring to a patent:
“For our studies, we used an LNP formulation proprietary to Acuitas Therapeutics described in US patent US10,221,127.”
A brief look at this patent suggests it may be a lipid with an amide-based head group, which would not be the same lipid used in these vaccines. How an amide head group alters the cationic nature, I am unsure. Additional links to other studies just continue to refer to other proprietary lipids, so I am not even sure if this is is a comparable lipid to the ones seen in the vaccines. I will withhold judgement for now, but keep this possible discrepancy in mind.
If it hasn’t been made clear, this paper feels all over the place tonally speaking. It feels like a paper that either side may point to in order to fit a narrative. The Title and the Summary alone feel a bit sensationalized, as if to allow readers to read into it what they want. Vaccine skeptics may view this study and say “see, we told you these things were dangerous!” while vaccine proponents may see it and say “see, these things are doing what they are supposed to! They are actually helping elicit a robust immune response!”. It feels like the researchers could have expanded so much more on the systemic inflammation aspect, but downplayed it and left it to nothing more than a wink and a nudge within the Discussion section.
The extent of biodegradation is up for debate, since esters don’t readily hydrolyze under acidic conditions without the aid of heat. Catalytic cleavage with the aid of enzymes may aid in the process. Again, the extent that this is occurring is unknown, and widespread distribution of the LNPs should raise questions about how much LNP is being degraded. It does raise questions as to whether factors of circulation should be utilized in order to provide a “first pass effect” of the LNPs to the liver before it can reach organs such as the heart and brain.



A question & heartfelt plea for you big brained re: neuroinvasion through the olfactory bulb• Healthy & unvaxxed, after prolonged exposure to my slightly covid-sick 18 yr old (home/quarantined from uni) I, of course, picked it up and had, untreated, only less than 24 hrs of a slight fever. However, I sustained total loss of my formerly incredibly sensitive olfactory senses. Over a yr later this loss has developed into the horrifying repugnant misrepresentation of many tastes and odors. I (wildly) suspect there is a connection to petroleum products having many notes and I can’t detect any but the base now? The citrusy perfume I always loved smells like axle grease as do many, many things taste now. I cannot bear eucalyptus, menthol, olive oil, sesame oil, arugula, red/green bell peppers, my old favorite moisturizer, etc… but most nightmarishly, myself! I am absolutely sickened by the smell of my own sweat. I’ve never been particularly sweaty & never used deodorant, always just powder, now I change my shirt 10X a day and I am self-conscious beyond words. I barely perspire but the tiniest bit is sickening to me. An Italian gardener and cook, I cannot smell flowers, I cannot smell what I’m cooking. after exposure to traffic or a restaurant kitchen I often smell a disgusting burning for days. For a while there, I thought maybe I was in ketosis and could only smell fat burning (this def’ly makes one crazy) but my diet though excellent is not that good and even if I don’t intermittent fast this is occurring and it seems to be getting worse. I take NAC, D& K, Quercetin, as I remember to. It is over a year now. Can you offer any wisdom or advice? A million thanks, blessings.
I have not had time to read this surely excellent analysis. I want to mention some things about inflammation which everyone should know.
There are multiple innate immune responses against viral, bacterial and fungal/yeast pathogens. However, these do not work much, or at all, against multicellular pathogens. Likewise, adaptive immune responses - the generation of antibodies, the antibodies themselves and the responses which destroy cells or viruses to which antibodies attach - work well on single cell and viral pathogen, but are not much use against multicellular pathogens.
So mammals (at least, I assume other vertebrates have it too) also have a gross cell-destroying set of immune responses which are capable of partly or completely destroying multicellular pathogens, AKA parasites. This is known as "inflammation". These inflammatory, indiscriminate, cell-destroying responses also may play some role in wound healing and in some responses to bacteria and viruses. However, they are primarily directed at parasites, such as helminths - intestinal worms.
For instance, eosinophils are the suicide bombers of the immune system. Their vacuoles contain enzymes which destroy DNA, RNA and proteins. When attracted to a site and triggered by inflammatory cytokines (signaling molecules released by immune cells, such as Th1 regulatory lymphocytes), the eosinophil disintegrates and lets loose its toxic payloads. Cells both of the host and the parasite are then destroyed, with other types of immune cells mopping up the debris.
There are numerous types of helminth. Many species of helminth have had it over us mammals for millions of years, so all our ancestors had one or more helminth infections for most of their lives. One way in which helminths have succeeded is by evolving the ability to exude compounds which downmodulate the host's inflammatory responses. There are an unknown number of these compounds, and at least two have been discovered. One is tuftsin-phosphorylcholine (TPC).
Hosts, including humans, have not evolved ways of ignoring these signaling molecules. Instead, our ancestors evolved _stronger_ inflammatory responses than are really needed, or healthy, to compensate for the ubiquitous down-modulation of such responses by one or more species of helminth. So without helminth infections, humans - with considerable individual genetic variation - are prone to having a stronger inflammatory response than is really healthy. This means that inflammation is often self-destructive. Sepsis is an obvious example. This kills 10 million people a year - and that was before COVID-19: https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(19)32989-7/fulltext
Just over a century ago, we in developed nations got rid of our helminths. We did the same for our companion and agricultural animals as well - and probably also for our lab rats and other non-human animals used by researchers.
This is the primary reason for the vast swath of overly inflammatory illnesses, many of them auto-immune - triggered by (adaptive) immune responses to our own cells.
So far, no-one has made any of these compounds available as drugs to suppress excessive inflammation, but some people find it best to suppress their psoriasis, rheumatoid arthritis, Crohn's disease, life-threatening asthma by deliberately being infected by one of several relatively benign helminths. See https://helminthictherapywiki.org .
To make matters _much_ worse, most humans have only a 1/2 to 1/10th of the 50 ng/mL (125 nmol/L = 1 part in 20,000,000 by mass) circulating 25-hydroxyvitamin D their immune systems need to function properly. https://vitamindstopscovid.info/05-mds/
25-hydroxyvitamin D is an essential input (raw material, it is not a signaling molecule in itself) for immune cells (most types, as best we know, but also other types not related to the immune system) to run their internal (intracrine. also known as "autocrine") signaling system, which plays a major role in individual cells being able to change their behaviour in response to their changing circumstances. (Some of the signaling molecule - 1,25-dihydroxyvitamin D - can also diffuse from these cells and affect the behaviour of other cells nearby, typically of different types. This is paracrine signaling.) See: https://vitamindstopscovid.info/02-autocrine/ .
So most humans have the double-whammy of lack of helminths and grossly inadequate vitamin D3 intakes (UV-B on the skin can make it too, but this damages DNA and so causes skin cancer - and there is very little in food or multivitamins) with resultant immune system dysregulation and general dysfunction due to lousy circulating 25-hydroxyvitamin D levels.
Virtually no researchers - including vitamin D researchers - recognise the problems caused by lack of helminths. Some vitamin D researchers are on the case of excessive inflammation - see Chauss et al. 2021 on Th1 regulatory lymphocytes from the lungs of hospitalised COVID-19 patients: https://aminotheory.com/cv19/icu/#2021-Chauss. However not one of them AFAIK discuss lack of helminths. Lots of researchers into inflammatory disorders (dozens or hundreds of disorders) don't think about either vitamin D or lack of helminths. The few people researching helminths and inflammation don't seem to think about lousy 25-hydroxyvitamin D levels.
Please bear all this in mind when discussing inflammation in humans, experimental animals (probably low vitamin D, surely without helminths) and our companion and agricultural animals. (Indoor agricultural animals often get decent vitamin D3 intakes - this is what most manufactured vitamin D3 cholecalciferol is used for. They die or do not produce food properly if they are deficient.)
For reasons unknown, higher than 50 ng/mL 25-hydroxyvitamin D levels can suppress the excessive inflammation of psoriasis, MS, rheumatoid arthritis etc. See the research articles cited at: https://vitamindstopscovid.info/06-adv/ - including those on helminths.
If most people had helminths and proper vitamin D3 intakes, such as 0.125 mg 5000 IU a day for 70 kg bodyweight, there would be a lot less trouble with excessive inflammation. Then these so-called vaccines against SARS-CoV-2 would probably cause less trouble, in some respects at least.
Then, there would be little reason to bother with such quasi-vaccines because few people infected with SARS-CoV-2 would become seriously ill. Those infected would shed less viruses in general and so overall rates of transmission would be very much lower than today - probably to the point of the disease not spreading very much.
However, 5000 IU a day is a gram every 22 years, and pharma grade vitamin D3 costs USD$2.50 a gram, ex-factory - so where's the profit in that??